Neuroendocrine tumours: choosing the best treatment
Which treatment(s) for which patient? Researchers from the universities of Geneva, Bern and Basel as well as from the HUG and Inselpital Bern performed systematic comparisons between the therapies available for neuroendocrine tumours in order to offer patients the most appropriate ones.
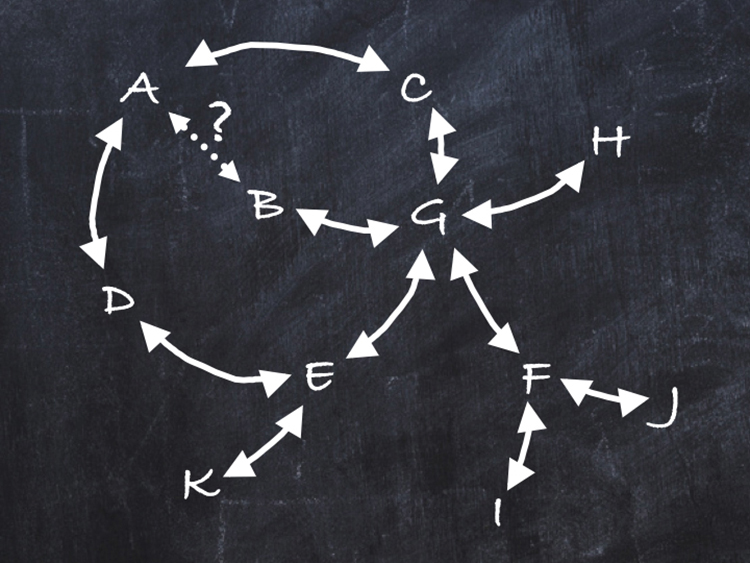
«The daily dilemma in medicine.» Eleven therapies are available for a given disease. Of the 55 possible direct comparisons between these therapies, only 11 have been performed. For a specific patient, treatments A and B appear to be the most suitable, but no direct comparison between these two treatments is available. Which one to choose, A or B? (Martin A. Walter , UNIGE)
An increasing number of new anti-cancer drugs are made available each year. During the authorization process, such new drugs usually undergo comparisons to one, but only rarely to multiple established drugs. This practice leads to a lack of comparisons between therapies, and makes it increasingly difficult for physicians to choose the best treatment for their patients. To address this, researchers at the Universities of Basel, Bern and Geneva and at the University Hospitals of Geneva (HUG) and Bern (Inselspital) have conducted an extensive comparison of all drugs used in the treatment of neuroendocrine tumours. Their study, to be read in JAMA Oncology, aims of guiding physicians through all available treatment options.
Neuroendocrine tumours can develop anywhere in the body from hormone-producing cells. Their prevalence is increasing and new therapies are regularly beefing up therapeutic options. “The growing number of new therapies constitutes a great opportunity, obviously. However, the fact that few comparative studies are carried out between these different drugs creates a dilemma for doctors when it comes to finding the best option for each patient,” says Martin A. Walter, Professor at the UNIGE Faculty of Medicine and Head of the Nuclear Medicine and Molecular Imaging Division at the HUG, who initiated and coordinated this study. “Indeed, it is actually sufficient to establish the superiority of a new molecule over a single established drug, or even over a placebo, to obtain approval from the regulatory authorities, and enter the market.”
“In such a situation, a network meta-analysis can be a valuable tool to generate indirect comparisons for therapies that have not yet been directly compared. They also make it possible to use all existing data to identify the most effective treatments,” adds Dr. Reto Kaderli, Head of Endocrine Surgery, Department of Visceral Surgery and Medicine ,Bern University Hospital and University of Bern, and first author of the study.
Independent research are less taken into account
Swiss researchers collaborated with Cochrane, a global organization that aims to facilitating clinical decision-making through systematic reviews of health interventions, and with researchers at McMaster University in Hamilton, Canada, where some of the key methodologies for the analysis of evidence-based medicine have been developed.
“One of the most striking results of our study is the high, and often underestimated, efficacy of combination therapies. And equally striking was that these combination therapies were underrepresented in international guidelines,” says Dr. Kaderli. Indeed, studies combining drugs produced by different pharmaceutical companies are mainly conducted by independent researchers, and their results are less taken into account in treatment guidelines than studies conducted by the pharmaceutical industry.
Success of nuclear medicine
“As a specialist in nuclear medicine, however, I am delighted with the promising results of our radioactive therapeutics,” says Professor Walter. Such a step still needs to be taken for surgical options, for which randomized controlled trials in combination with other therapies are still lacking. “Our work thus marks an important step in the search for the best therapeutic option for patients with neuroendocrine tumours, and highlights the need for independent evidence-based medicine,” conclude the authors.
14 Feb 2019