Is schizophrenia the cost of a poor brain optimisation?

Patients with 22q11.2 deletion syndrome have a high risk of developing schizophrenia. According to a recent study by neuroscientists from Synapsy, the Swiss National Research Centre of Competences in Research into Mental Illness, their brains seems to use energy in a non-optimal fashion when thinking.
Knowing how much energy the brain consumes for thinking has always been a source of heated debate in the neuroscientific community. The reason is simple: the brain is a very energy-intensive organ, and almost all cerebral pathologies are linked, directly or indirectly, to cerebral energy metabolism. Psychosis is a term used in psychiatry to refer to an abnormal state of mind – and, by extension, of thinking – that typically appears in psychiatric disorders such as schizophrenia. Consequently, the task is particularly difficult since thinking (whether psychotic or not) involves several states of brain activity and, it follows, a huge number of interdependent neural networks.
In spite of the obvious difficulty, Daniela Zöller, who was supported by Synapsy’s research fund for her PhD and postdoctoral research conjointly at the laboratory of Stephan Eliez, UniGE, and the one of Dimitri Van De Ville, EPFL and UniGE, set out to understand whether people at risk of developing schizophrenia had a defect in the energy states associated with thinking. “Schizophrenia is a brain development disorder”, she begins. “It doesn’t manifest itself until adolescence or the onset of adulthood. Detecting early markers of the disorder before it develops could help to prevent it.” This is why the neuroscientist focused on patients with 22q11.2 deletion syndrome – a genetic defect that increases the risk of developing schizophrenia – in a study published in the scientific journal Human Brain Mapping.
The energy states involved in thinking
Dr Zöller and her colleagues used structural and functional magnetic resonance imaging (MRI) to visualise the different networks activated by thinking. They did this by simply placing a person in an MRI and asking him or her to do nothing, leaving a space free for thoughts to emerge. They observed while regions of the brain activated dynamically and coordinated with each other, reflecting several states of thought, as Dr Zöller explains: “It’s possible to estimate the energy needed to switch between states using theoretical mathematical models that are well described in the scientific literature”. The energy cost of states of thinking can then be estimated theoretically using imaging to look at the structure and connectivity of the neural networks.
Unprofitable psychotic thoughts
Dr. Zöller benefitted from the multidisciplinary environment in the labs of Dimitri Van De Ville, Synapsy researchers Marie Schaer and Stephan Eliez, as well as research stays to the lab of Danielle Bassett at the University of Pennsylvania, to fully exploit the imaging data of healthy individuals and patients suffering from 22q11.2 deletion syndrome. The study focused on data from the entire brain rather than single regions. “We’re talking about 17 different states of brain activity that are spread across the brain and that overlap,” says Dr Zöller, before continuing: “We found that 22q11.2 patients engage in a shorter period of time in brain states that require higher energy.” This data suggests that 22q11.2 patients might use their brains in a less cost-effective manner. It’s a discovery that orients our understanding of the mechanisms that underlie vulnerability to psychosis. Since only about 1% of all people with schizophrenia have a 22q11 deletion syndrome, authors of the study recommend not to generalize the findings to schizophrenia at-large, with Dr Zöller concluding, “ Now we need but to confirm and extend these important observations for the understanding of schizophrenic-type disorders.”
By Yann Bernardinelli, Press Officer NCCR-Synapsy
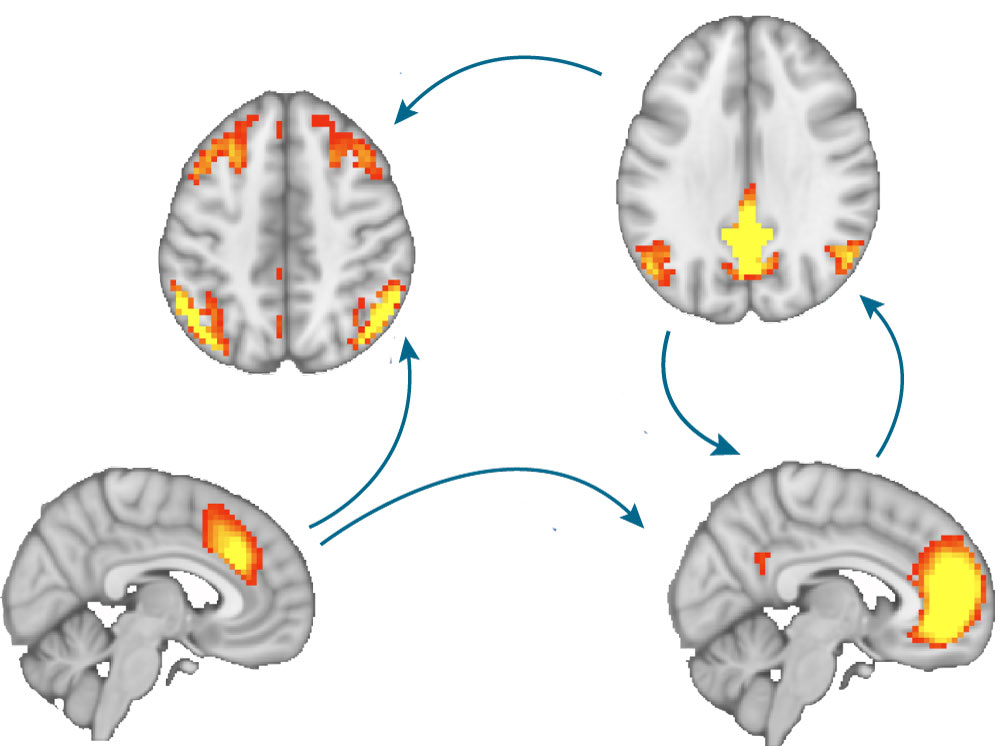
Caption: Different brain states measured by MRI when a patient is at rest. @ EPFL / Zöller
6 Apr 2021