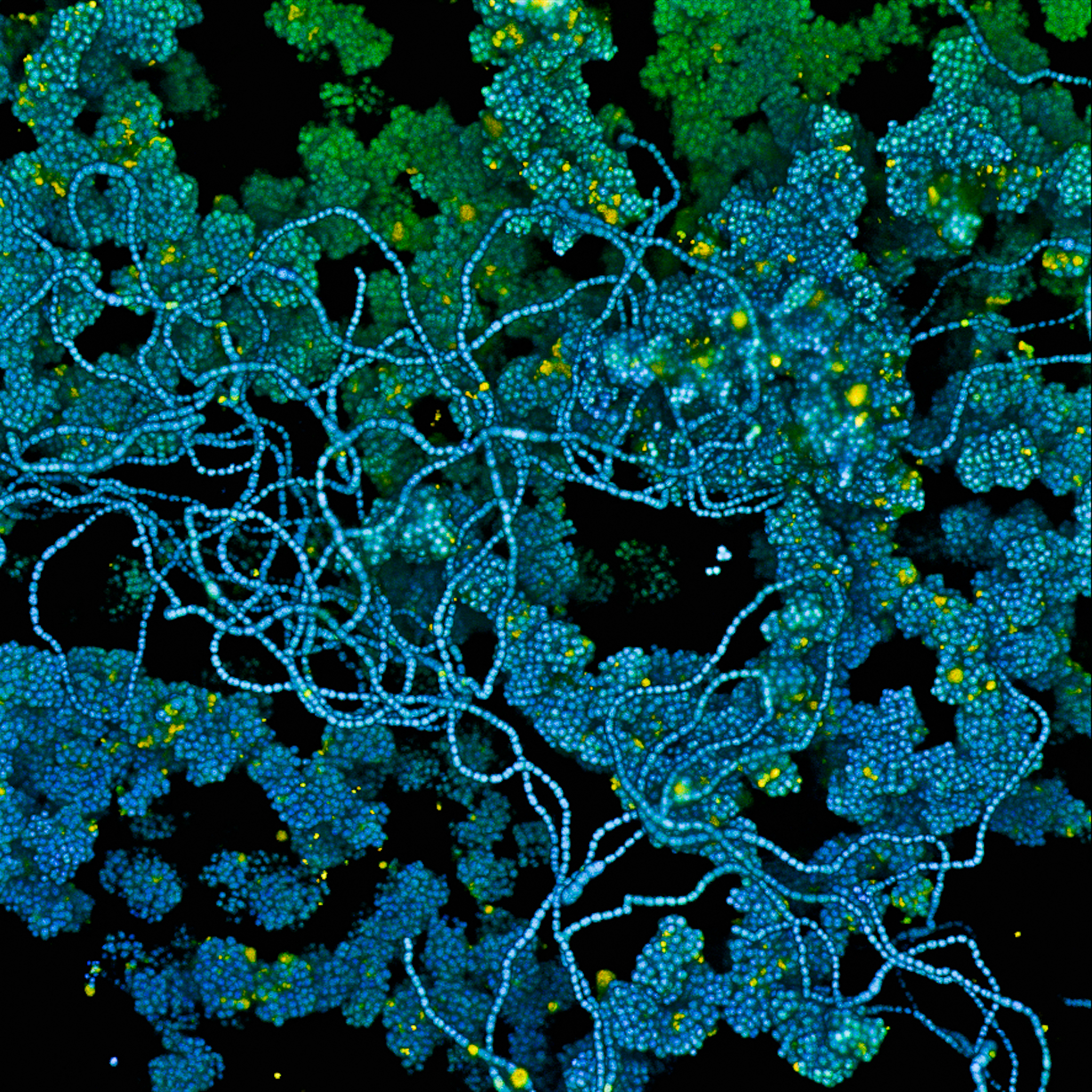
[1044] Pathogenesis of biofilm-associated infections
Biofilms contribute to the majority of chronic infections, which are difficult to treat due to an intrinsic antibiotic tolerance of biofilm bacteria. The polymicrobial nature of many biofilm-associated infections can further amplify antibiotic tolerance within the infection-associated bacterial community. Enterococci are common members of the healthy gut microbiome. Enterococci are also a leading cause of hospital-acquired, biofilm-associated, infections of the urinary tract, wounds, and dysbiotic gut. Despite the prevalence of Enterococci in biofilm-associated infections, the mechanisms by which these organisms generate and persist within biofilms during infection are not well-understood. Our research tackles this knowledge gap by asking three simple questions: 1) How do Enterococci sense and respond the disparate host and microbial environments encountered during infection, in order to build biofilms that are most suitable for each infection site? 2) How do infection-relevant polymicrobial interactions contribute to biofilm-associated infection? 3) How are Enterococci able to subvert the mammalian immune response to persist during acute and chronic biofilm-associated infections? Insights from this work will provide fundamental knowledge of Enterococcal pathways or factors that may be targeted for future intervention strategies to prevent or eradicate infection.